1. Failure to Capture- Pulse sent but myocardium doesn’t feel it. No depolarization. If myocardium is in refractory state, depolarization won’t happen. 1.Causes include electrode displacement, wire fracture, electrolyte disturbance, medications, heart disease, MI, or exit block.
2.N.B. If native rate above pacemaker threshold, it naturally won’t send a signal. That’s not failure to capture.
3.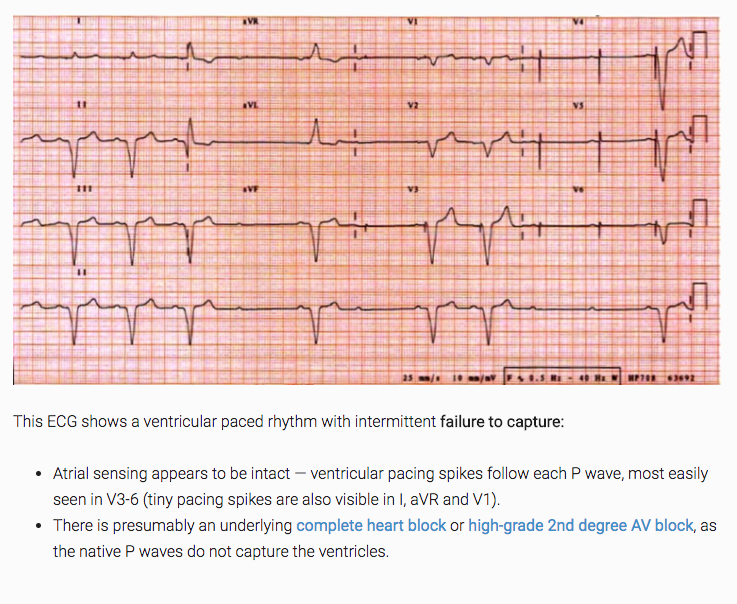 from LITFL!
from LITFL!
2. Failure to Pace- Pacemaker not sending a pulse to stimulate the heart. HR found below the lower limit set on the device and no pacemaker artifact on EKG.
1.Pacemaker over-sensing is most common cause of failure to pace.
2.Lead fracture from blunt trauma due to MVA, sports, or falls
3.Over-sensing caused by device misinterpretation of myopotentials from surrounding muscle (e.g. someone painting a room, causing contraction of the pectoris). Can also be due to retrograde p waves, t waves, or other post-depolarization electrical activity sensing as though it was a normal potential and causing the pacemaker not to send a stimulus.
4.OVER SENSE=FAILURE TO PACE
5.May see large P or T waves, skeletal muscle activity on EKG or may not see anything. If patient stimulates rectus or pectoral muscle while on cardiac monitor, may see reduced pacemaker output.
3. Failure to Sense- Pacemaker doesn’t recognize a myocardial depolarization (native activity) after it’s traveled up the lead wire.
1.“Blanking” where the pacer doesn’t sense a normal depolarization. Prolonged refractory period can be 2/2 changes in the patient’s EKG complex (e.g. new BBB) and cause functional UNDER-sensing. Usually lead fracture or insulation defects.
1.May see pacing spikes WITHIN the QRS complex.
2.Get asyncronous pacing
3.UNDER SENSE = FAILURE TO SENSE
2.Causes: increased stimulation threshold at electrode site (exit block), poor lead contact/fracture/insulation defects, new BBB or programming problems
http://www.emdocs.net/pacemaker-and-aicd-management-in-the-emergency-department/
Rosen’s Chapter 70: Implantable Cardiac Devices
https://lifeinthefastlane.com/ecg-library/pacemaker-malfunction/
