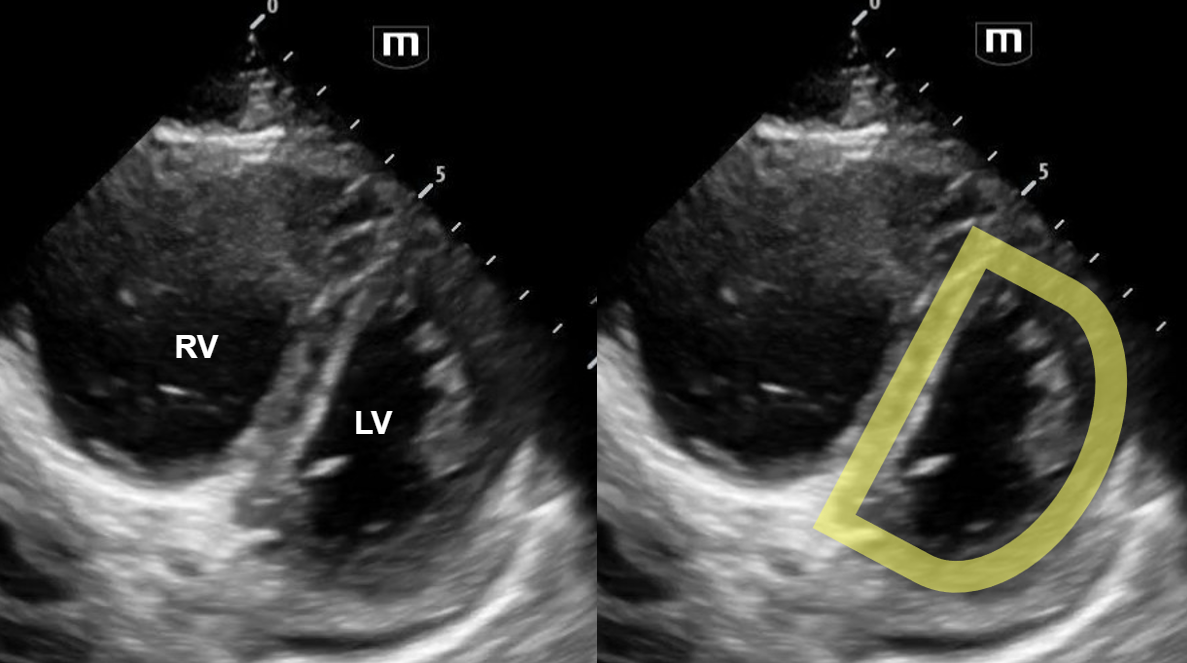
Happy Tuesday! I hope you all enjoyed your Labor Day Weekend.
For this week’s trauma Tuesday topic, I wanted to discuss Tasers. In the past 2 years I have seen a handful of patients in NYPD custody in need of medical checks as a result of being tased.
Taser guns were first developed in the 1970’s. The name is actually an acronym which stands for Tom A. Swift Electric Rifle. The inventor, Jack Cover, was a huge fan of the science fiction book series featuring the main character Tom Swift. The Taser was introduced for use by law enforcement in the 1990s. It falls under the category of less-lethal weapons which also includes batons, mace, tear gas, and projectiles like foam rounds.
The Taser is a type of Conducted Electrical Weapon. Pulling the trigger releases the compressed nitrogen. The 2 pronged darts that are attached to a copper wire fire out. As the darts make contact with skin, the electrical circuit is completed and electricity courses through. As it does, it causes painful involuntary muscle contraction.
As of 2019, the American Academy of Emergency Medicine does not recommend routine workup in an otherwise well appearing and asymptomatic individual who was exposed to less than 15 seconds of electrical current. No need for EKG’s, laboratory testing or observation. There has been little evidence showing significant medical harm or physiologic change in patients who have received a Taser shock, even in those who have underlying cardiac abnormalities or defibrillators.
It is important to assess the skin and area that was struck by the prongs. Those can cause minor burns and skin injury. There have been isolated case reports of the metal barbs causing penetration injuries as well. This is a case study where a patient had a barb stuck in his penis. Also consider other injuries that someone may sustain if they had gotten tased and fallen onto the ground.
References
https://www.aaem.org/statements/evaluations-after-a-taser-device-activation/
Baliatsas C, Gerbecks J, Dückers MLA, Yzermans CJ. Human Health Risks of Conducted Electrical Weapon Exposure: A Systematic Review. JAMA Netw Open. 2021 Feb 1;4(2):e2037209. doi: 10.1001/jamanetworkopen.2020.37209. PMID: 33576818; PMCID: PMC7881359.
Theisen K, Slater R, Hale N. Taser-Related Testicular Trauma. Urology. 2016 Feb;88:e5. doi: 10.1016/j.urology.2015.11.011. Epub 2015 Dec 1. PMID: 26592466.
Bralow LM. Misfire: A man with genital trauma. J Am Coll Emerg Physicians Open. 2022 Dec 21;3(6):e12875. doi: 10.1002/emp2.12875. PMID: 36570370; PMCID: PMC9772490.